Why GLP‑1 Injection Therapy Is a Game‑Changer
GLP‑1 (glucagon‑like peptide‑1) is a gut hormone that boosts insulin, slows gastric emptying, and signals satiety in the brain. Synthetic GLP‑1 receptor agonists such as semaglutide (Wegovy®) and tirzepatide (Zepbound®) have been FDA‑approved for chronic weight management in adults with a BMI ≥ 30 kg/m² or ≥ 27 kg/m² with a weight‑related condition.
Integrative health programs weave this pharmacology into a whole‑person plan: clinicians pair the weekly sub‑Q injection with personalized nutrition, resistance‑training, mindfulness‑based stress reduction, and behavioral coaching. By addressing hormone pathways, gut microbiome, sleep, and emotional eating, the therapy aligns with the mind‑body connection that integrative medicine champions.
Beyond weight loss, GLP‑1 agents improve blood pressure, lipid profiles, and glycemic control, lower the risk of progressing to type 2 diabetes, and may confer cardiometabolic and kidney benefits. When combined with balanced diet and activity, they become a powerful, patient‑centered tool for sustainable health transformation.
GLP‑1 Weight Loss for Non‑Diabetics
| Outcome | Weight Loss % (average) | Duration | Key Points |
|---|---|---|---|
| Clinical Trials | 10‑20 % | 68 weeks | Paired with nutrition & activity |
| Real‑World Cohort (367 k pts) | 10‑20 % | Variable | Mild‑to‑moderate GI effects most common |
| Dual‑Agonist (tirzepatide) | Up to 22.5 % | Ongoing studies | Long‑term safety in non‑diabetics under investigation |
| Triple‑Agonist candidates | TBD | TBD | Early phase; efficacy promising, safety unknown |
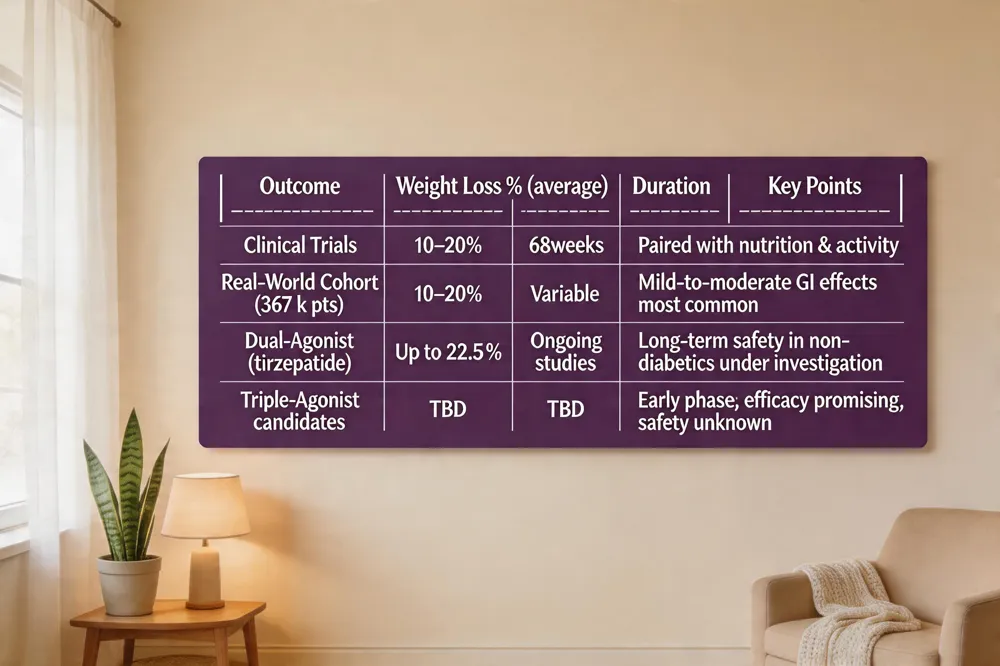 GLP‑1 receptor agonists such as semaglutide (Wegovy) and liraglutide (Saxenda) mimic the gut hormone GLP‑1, slowing gastric emptying, enhancing satiety signals in the hypothalamus, and improving insulin sensitivity—all without needing a diabetic glucose‑control target. In adults who are overweight or obese but do not have diabetes, clinical trials consistently show 10‑20 % body‑weight loss after 68 weeks when the medication is paired with balanced nutrition and regular activity. Real‑world data from a cohort of 367 000 non‑diabetic patients confirm robust efficacy and reveal a safety profile dominated by mild‑to‑moderate gastrointestinal effects (nausea, vomiting, diarrhea, constipation) that usually subside after dose titration. Rare events such as delayed gastric emptying or gallstones occur at low rates. Emerging dual‑agonists (e.g., tirzepatide) and triple‑agonist candidates aim to amplify appetite suppression and metabolic benefits, but long‑term safety in non‑diabetic populations remains under investigation. Under physician‑supervised, integrative care—combining medication, personalized nutrition, activity, and mind‑body support—GLP‑1 therapy offers a promising, patient‑centered pathway to sustainable weight loss.
GLP‑1 receptor agonists such as semaglutide (Wegovy) and liraglutide (Saxenda) mimic the gut hormone GLP‑1, slowing gastric emptying, enhancing satiety signals in the hypothalamus, and improving insulin sensitivity—all without needing a diabetic glucose‑control target. In adults who are overweight or obese but do not have diabetes, clinical trials consistently show 10‑20 % body‑weight loss after 68 weeks when the medication is paired with balanced nutrition and regular activity. Real‑world data from a cohort of 367 000 non‑diabetic patients confirm robust efficacy and reveal a safety profile dominated by mild‑to‑moderate gastrointestinal effects (nausea, vomiting, diarrhea, constipation) that usually subside after dose titration. Rare events such as delayed gastric emptying or gallstones occur at low rates. Emerging dual‑agonists (e.g., tirzepatide) and triple‑agonist candidates aim to amplify appetite suppression and metabolic benefits, but long‑term safety in non‑diabetic populations remains under investigation. Under physician‑supervised, integrative care—combining medication, personalized nutrition, activity, and mind‑body support—GLP‑1 therapy offers a promising, patient‑centered pathway to sustainable weight loss.
Choosing the Right Medication: OTC vs Prescription
| Option | FDA Status | Mechanism | Typical Weight Loss | Notes |
|---|---|---|---|---|
| Alli (orlistat) | OTC 60 mg | Intestinal lipase inhibitor | ~5‑6 lb (~2‑3 kg) after 1 yr | Reduces fat‑soluble vitamin absorption → multivitamin needed |
| Semaglutide (Wegovy) | Prescription | GLP‑1 receptor agonist – slows gastric emptying, ↑ satiety | 15‑20 % (up to 22 % in trials) | BMI ≥ 30 kg/m² or ≥ 27 kg/m² + comorbidity |
| Liraglutide (Saxenda) | Prescription | GLP‑1 receptor agonist – similar to semaglutide | 5‑10 % | Daily injection |
| Phentermine‑Topiramate (Qsymia) | Prescription | Appetite suppression + neuro‑modulation | 8‑10 % | Contraindicated in pregnancy |
| Bupropion‑Naltrexone (Contrave) | Prescription | Dopamine‑noradrenaline & opioid receptor modulation | 5‑10 % | May increase blood pressure |
| Oral Semaglutide (Wegovy Pill) | Prescription | GLP‑1 receptor agonist (oral) | 10‑15 % | Requires fasting before dose |
 When you consider weight‑loss options, the only FDA‑approved over‑the‑counter (OTC) drug is Alli (60 mg orlistat). It blocks intestinal lipase, leading to modest loss—about 5‑6 lb after a year—when paired with a low‑fat, calorie‑controlled diet and regular activity. Because it reduces absorption of fat‑soluble vitamins, a multivitamin taken two hours after the dose is advisable, and a healthcare professional should review its suitability.
When you consider weight‑loss options, the only FDA‑approved over‑the‑counter (OTC) drug is Alli (60 mg orlistat). It blocks intestinal lipase, leading to modest loss—about 5‑6 lb after a year—when paired with a low‑fat, calorie‑controlled diet and regular activity. Because it reduces absorption of fat‑soluble vitamins, a multivitamin taken two hours after the dose is advisable, and a healthcare professional should review its suitability.
For abdominal fat specifically, no single prescription pill works for everyone. FDA‑approved agents such as semaglutide (Wegovy), liraglutide (Saxenda), phentermine‑topiramate (Qsymia), and bupropion‑naltrexone (Contrave) each target appetite, satiety, or nutrient absorption through distinct mechanisms. The best choice hinges on your BMI, comorbidities (e.g., diabetes, hypertension), and tolerance for side effects, making a clinician‑guided evaluation essential.
GLP‑1 drugs officially approved for weight loss include injectable semaglutide (Wegovy), oral semaglutide (Wegovy Pill), tirzepatide (Zepbound), and liraglutide (Saxenda). They mimic the natural hormone GLP‑1, slowing gastric emptying and increasing fullness, and are prescribed for adults with a BMI ≥ 30 kg/m² or ≥ 27 kg/m² with weight‑related conditions. Ongoing medical supervision, lifestyle counseling, and mindful eating are critical to maximize benefits and sustain results.
Dosage, Administration, and Safety of GLP‑1 Injections
| Medication | Starting Dose | Titration Schedule | Injection Site | Common Side Effects | Rare Serious Risks |
|---|---|---|---|---|---|
| Semaglutide (Wegovy) | 0.25 mg weekly | ↑ by 0.25 mg every 4 wk to 1.0 mg (or higher) | Abdomen, thigh, upper arm (rotate weekly) | Nausea, vomiting, diarrhea, constipation | Pancreatitis, gallbladder disease, thyroid C‑cell tumors |
| Tirzepatide (Zepbound) | 2.5 mg weekly | ↑ by 2.5 mg every 4 wk to 10‑15 mg | Same as above | GI upset, headache | Same as above, plus potential hypoglycemia if combined with insulin |
| Liraglutide (Saxenda) | 0.6 mg daily | ↑ by 0.6 mg weekly to 3.0 mg | Abdomen, thigh, upper arm (rotate) | Nausea, injection site reactions | Pancreatitis, thyroid tumors |
 Injection technique is subcutaneous, using the abdomen, thigh, or upper arm. Rotate sites weekly to avoid lipohypertrophy; pinch a 1‑inch fold of fatty tissue, clean with alcohol, insert at 90°, and hold the needle for 5‑10 seconds. Common side effects are mild GI upset; rare but serious events include pancreatitis, gallbladder disease, and thyroid C‑cell tumors, especially in those with a personal or family history of medullary thyroid carcinoma or MEN 2. Ongoing monitoring by a multidisciplinary team—physician, dietitian, and wellness coach—ensures safety, supports nutrition, and preserves muscle mass during GLP‑1 therapy.
Injection technique is subcutaneous, using the abdomen, thigh, or upper arm. Rotate sites weekly to avoid lipohypertrophy; pinch a 1‑inch fold of fatty tissue, clean with alcohol, insert at 90°, and hold the needle for 5‑10 seconds. Common side effects are mild GI upset; rare but serious events include pancreatitis, gallbladder disease, and thyroid C‑cell tumors, especially in those with a personal or family history of medullary thyroid carcinoma or MEN 2. Ongoing monitoring by a multidisciplinary team—physician, dietitian, and wellness coach—ensures safety, supports nutrition, and preserves muscle mass during GLP‑1 therapy.
Accessing GLP‑1 Therapy: Online Prescriptions, Purchasing, and Insurance
| Step | Description | Who Involved | Typical Timeframe |
|---|---|---|---|
| 1️⃣ Eligibility Review | Video/phone visit, BMI & health history check | Licensed clinician | 15‑30 min |
| 2️⃣ Prescription Issuance | Electronic prescription sent to pharmacy | Clinician | Immediately after visit |
| 3️⃣ Pharmacy Fill | Fill at national chain or local pharmacy | Pharmacist | Same‑day to 2 days |
| 4️⃣ Delivery (optional) | Direct‑to‑door shipping via tele‑health service | Pharmacy/Logistics | 3‑5 days |
| 5️⃣ Follow‑up | Monthly virtual check‑ins for weight, side‑effects, dose | Clinician, dietitian, coach | Every 4 weeks |
| 6️⃣ Insurance/Assistance | Prior authorization, patient‑assist programs | Insurance rep, manufacturer | 1‑3 weeks for approval |
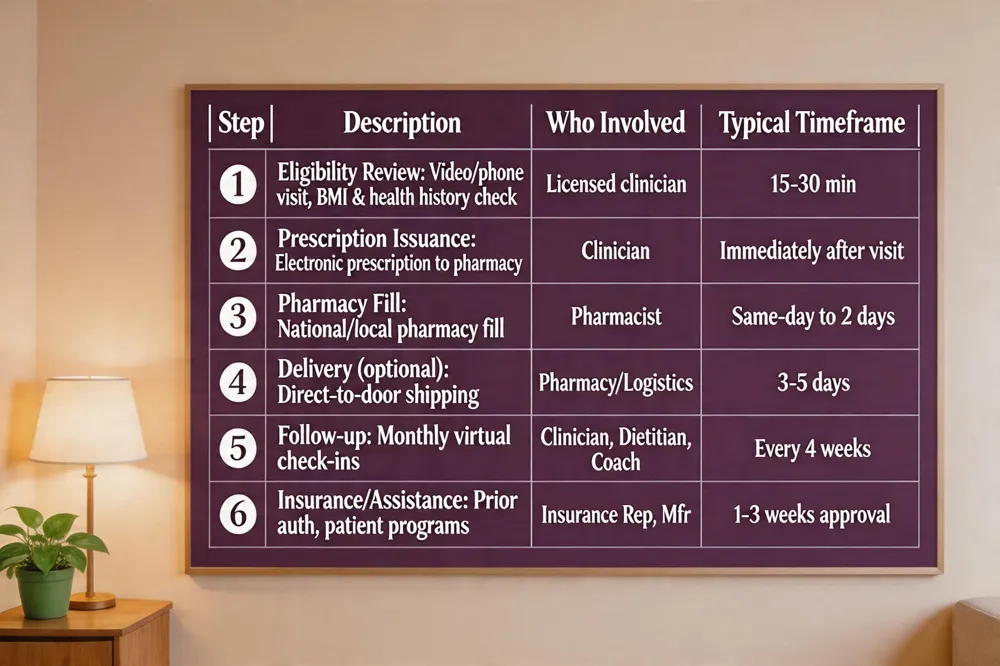 Virtual care workflow for GLP‑1 prescriptions – Obtaining a GLP‑1 prescription online begins with a video or phone visit with a licensed clinician. The provider reviews your medical history, BMI (≥30 kg/m² or ≥27 kg/m² with a related condition), and any weight‑related health issues. If you meet eligibility criteria, the clinician issues an electronic prescription for a GLP‑1 agonist such as semaglutide (Wegovy®/Ozempic®), tirzepatide (Zepbound®), or liraglutide (Saxenda®). Follow‑up appointments are usually scheduled monthly to monitor weight, side‑effects, and dose adjustments, ensuring safe, personalized care without needing an in‑person visit.
Virtual care workflow for GLP‑1 prescriptions – Obtaining a GLP‑1 prescription online begins with a video or phone visit with a licensed clinician. The provider reviews your medical history, BMI (≥30 kg/m² or ≥27 kg/m² with a related condition), and any weight‑related health issues. If you meet eligibility criteria, the clinician issues an electronic prescription for a GLP‑1 agonist such as semaglutide (Wegovy®/Ozempic®), tirzepatide (Zepbound®), or liraglutide (Saxenda®). Follow‑up appointments are usually scheduled monthly to monitor weight, side‑effects, and dose adjustments, ensuring safe, personalized care without needing an in‑person visit.
Where to obtain medication – Prescription GLP‑1 medications can be filled at any pharmacy that accepts the electronic prescription—national chains like Walgreens, CVS, Walmart, or local independent pharmacies. Walgreens Weight Management offers a streamlined tele‑health option that evaluates eligibility and ships the medication directly to your door. Over‑the‑counter supplements claiming to “boost GLP‑1” are not FDA‑approved and should not replace a prescription‑based regimen.
Insurance coverage, Medicaid, and Medi‑Cal specifics – Most commercial insurers, Medicare, and Medicaid treat GLP‑1 injectables as specialty drugs and require prior authorization, a documented obesity‑related comorbidity, and a high BMI. Medicare generally does not cover them for weight loss alone. Manufacturer discount programs and patient‑assistance resources can offset out‑of‑pocket costs. Medi‑Cal may cover medically‑necessary weight‑loss services, including GLP‑1 therapy, when prescribed for diabetes or other approved indications, but coverage for weight‑loss‑only use is limited and requires physician documentation and prior authorization.
Patients should verify their specific plan details, appeal denials when needed, and work with a multidisciplinary team—dietitians, health coaches, and integrative practitioners—to combine medication with nutrition, activity, and stress‑management for sustainable results.
Top Medically Supervised Weight‑Loss Programs & Finding Local Clinics
| Program / Clinic | Primary Location(s) | Core Services | Insurance Acceptance |
|---|---|---|---|
| Northwestern Medicine – Center for Lifestyle Medicine | Chicago, IL | GLP‑1 therapy, diet, exercise, behavioral health | Major commercial plans |
| UChicago Medicine – Weight Loss Clinic | Chicago, IL | Multidisciplinary team, GLP‑1, surgical options | Medicare, Medicaid, private |
| Abbott Northwestern Hospital | Minneapolis, MN | Comprehensive obesity medicine, GLP‑1, bariatric surgery | Broad coverage |
| Baylor St. Luke’s | Dallas, TX | Integrated GLP‑1, nutrition, fitness coaching | Private & Medicare |
| AZ Weight‑Loss Clinic | Phoenix, AZ | GLP‑1, personalized nutrition, mind‑body | Most plans |
| Nowak Aesthetics | Chula Vista, CA (San Diego area) | Semaglutide injections, labs, coaching | Private only (cash pay) |
| Beauty Lounge Medical Spa | San Marcos, Hillcrest, Temecula, CA | Weekly GLP‑1 injections, aesthetic services | Cash or private |
| La Jolla Cosmetic Surgery Centre | La Jolla/Carlsbad, CA | GLP‑1 therapy, surgical & non‑surgical options | Private & select insurers |
 Leading U.S. weight‑loss centers blend multidisciplinary medical care with holistic lifestyle support. Programs such as Northwestern Medicine’s Center for Lifestyle Medicine, UChicago Medicine’s Weight Loss Clinic, and the nationally recognized America’s Best Weight‑Loss Clinics 2025 (e.g., Abbott Northwestern Hospital, Baylor St. Luke’s, AZ Weight‑Loss Clinic) employ obesity‑medicine physicians, registered dietitians, exercise specialists, and behavioral therapists. They begin with a thorough medical evaluation to uncover hormonal, medication‑related, or metabolic contributors, then prescribe FDA‑approved GLP‑1 agonists (semaglutide, tirzepatide) alongside balanced nutrition, mindful eating, and personalized physical activity plans.
Leading U.S. weight‑loss centers blend multidisciplinary medical care with holistic lifestyle support. Programs such as Northwestern Medicine’s Center for Lifestyle Medicine, UChicago Medicine’s Weight Loss Clinic, and the nationally recognized America’s Best Weight‑Loss Clinics 2025 (e.g., Abbott Northwestern Hospital, Baylor St. Luke’s, AZ Weight‑Loss Clinic) employ obesity‑medicine physicians, registered dietitians, exercise specialists, and behavioral therapists. They begin with a thorough medical evaluation to uncover hormonal, medication‑related, or metabolic contributors, then prescribe FDA‑approved GLP‑1 agonists (semaglutide, tirzepatide) alongside balanced nutrition, mindful eating, and personalized physical activity plans.
A broader landscape includes physician‑guided calorie‑deficit programs, commercial curricula like WW, Nutrisystem, Noom, and diet‑specific approaches (Mediterranean, low‑carb, plant‑based). Many clinics integrate GLP‑1 therapy into these plans, offering tele‑health coaching, group classes, and mind‑body techniques such as yoga or acupuncture.
To locate a clinic, search “weight‑loss clinic + your city/ZIP,” review services (medical supervision, dietitian access, medication management), verify insurance coverage, and confirm a multidisciplinary team.
In San Diego, reputable semaglutide options include Nowak Aesthetics (Chula Vista), Beauty Lounge Medical Spa (San Marcos, Hillcrest, Temecula), and La Jolla Cosmetic Surgery Centre (La Jolla/Carlsbad), each requiring an initial evaluation and lab work before initiating weekly injections or oral dosing.
Integrative & Holistic Approaches to Sustainable Weight Loss
| Component | Description | Evidence Base |
|---|---|---|
| Personalized Nutrition | Dietitian‑crafted meal plans (Mediterranean, low‑carb, plant‑based) | RCTs show improved adherence & weight loss |
| Mind‑Body Practices | Mindfulness, yoga, stress‑reduction coaching | Meta‑analyses link stress reduction to lower intake |
| Functional‑Medicine Testing | Gut microbiome, hormone panels, nutrient status | Emerging data on metabolic optimization |
| Prescription‑Grade Meal Replacements | Clinically formulated shakes or bars | FDA‑cleared for medical nutrition therapy |
| Targeted Supplements | GLP‑1 boosters (research‑grade), fiber, probiotics | Limited; used as adjuncts |
| Physical Activity Coaching | Structured aerobic + resistance programs | ACSM guidelines support synergistic weight loss |
 Integrative and holistic weight‑loss programs view each client as a whole person, blending personalized nutrition plans crafted by registered dietitians with evidence‑based medical interventions such as prescription‑grade meal replacements, appetite‑suppressing GLP‑1 agonists, and targeted supplements. Mind‑body connection is addressed through stress‑reduction techniques, mindfulness coaching, and behavioral therapy that reshape emotional eating triggers. Functional‑medicine testing, gut‑health optimization, and detoxification protocols uncover hidden metabolic imbalances, while regular physical‑activity guidance and lifestyle coaching foster sustainable habits beyond the clinic walls.
Integrative and holistic weight‑loss programs view each client as a whole person, blending personalized nutrition plans crafted by registered dietitians with evidence‑based medical interventions such as prescription‑grade meal replacements, appetite‑suppressing GLP‑1 agonists, and targeted supplements. Mind‑body connection is addressed through stress‑reduction techniques, mindfulness coaching, and behavioral therapy that reshape emotional eating triggers. Functional‑medicine testing, gut‑health optimization, and detoxification protocols uncover hidden metabolic imbalances, while regular physical‑activity guidance and lifestyle coaching foster sustainable habits beyond the clinic walls.
Weight loss programs without medication rely on sustainable lifestyle changes. The Mayo Clinic Diet’s two‑phase approach (initial “Lose It!” followed by lifelong “Live It!”), the NIDDK‑recommended reduced‑calorie, nutrient‑dense eating plan, and regular aerobic activity provide a proven framework. Integrative providers add personalized coaching, stress‑management, and detoxification to address mental and emotional factors.
Free evidence‑based weight‑loss resources include the Mayo Clinic Diet’s free online assessment, the NHS 12‑week Weight Loss Plan app, and the UK NHS Digital Weight Management Programme, all offering peer‑reviewed, no‑cost guidance for adults seeking a holistic, personalized path to lasting weight loss.
Personalizing Treatment: Discussing Medications and Choosing the Strongest Options
| Medication | Avg Weight Loss % (clinical) | Primary Indication | Key Considerations |
|---|---|---|---|
| Semaglutide (Wegovy) | 15‑20 % (up to 22 % in some trials) | BMI ≥ 30 kg/m² or ≥ 27 kg/m² + comorbidity | Injection weekly, GI side‑effects |
| Tirzepatide (Zepbound) | 20‑22.5 % | Same as above | Dual GLP‑1/GIP agonist, higher efficacy, similar safety |
| Liraglutide (Saxenda) | 5‑10 % | BMI ≥ 30 kg/m² or ≥ 27 kg/m² + comorbidity | Daily injection, modest effect |
| Phentermine‑Topiramate (Qsymia) | 8‑10 % | BMI ≥ 30 kg/m² | May raise blood pressure, not for pregnancy |
| Bupropion‑Naltrexone (Contrave) | 5‑10 % | BMI ≥ 30 kg/m² | Mood effects, watch for seizures |
| Orlistat (Alli) | 2‑3 % (≈5‑6 lb) | OTC option | Fat‑soluble vitamin loss, GI side‑effects |
 The most potent prescription weight‑loss drugs available today are the GLP‑1 receptor agonists—semaglutide (Wegovy) and the dual GLP‑1/GIP agonist tirzepatide (Zepbound). Clinical trials show average weight reductions of 15‑20 % (up to 22.5 % for tirzepatide), far exceeding older agents such as phentermine or orlistat. Choosing the “strongest” medication depends on your BMI, comorbidities, insurance, and tolerance of side effects, so a provider will tailor the prescription accordingly.
The most potent prescription weight‑loss drugs available today are the GLP‑1 receptor agonists—semaglutide (Wegovy) and the dual GLP‑1/GIP agonist tirzepatide (Zepbound). Clinical trials show average weight reductions of 15‑20 % (up to 22.5 % for tirzepatide), far exceeding older agents such as phentermine or orlistat. Choosing the “strongest” medication depends on your BMI, comorbidities, insurance, and tolerance of side effects, so a provider will tailor the prescription accordingly.
Overall, the most effective medical treatments combine FDA‑approved drugs (GLP‑1 agonists, bupropion‑naltrexone, phentermine‑topiramate, orlistat) with a personalized nutrition plan, regular physical activity, and behavioral counseling. These therapies are typically reserved for adults with a BMI ≥ 30 kg/m² or a BMI ≥ 27 kg/m² with obesity‑related conditions, and they should be monitored by a qualified healthcare professional for safety and optimal results.
Maintaining Success: Lifestyle, Monitoring, and Long‑Term Strategies
| Pillar | Key Actions | Frequency | Benefits |
|---|---|---|---|
| Nutrition | 0.8‑1.2 g protein/kg, high fiber, healthy fats | Every meal | Preserves lean mass, satiety |
| Physical Activity | Resistance training 2‑3 × wk + aerobic 150 min / wk | Weekly/Monthly | Maintains muscle, improves metabolism |
| Professional Support | Monthly visits with physician, dietitian, coach | Monthly | Early detection of side‑effects, accountability |
| Monitoring | Track weight, BP, labs (glucose, lipids, liver) | Every 4‑8 weeks | Adjust dose, ensure safety |
| Lifestyle Adjustment | Mindfulness, sleep hygiene, stress management | Daily | Reduces emotional eating, improves adherence |
 Sustaining the weight‑loss gains achieved with GLP‑1 therapy hinges on three pillars. First, a nutrition plan rich in lean protein ( 0.8‑1.2 g/kg body weight daily), fiber, and healthy fats helps preserve muscle mass while the medication slows gastric emptying and curbs appetite. Second, regular physical activity—especially resistance training 2‑3 times per week—maintains lean body mass, supports metabolic health, and counteracts the modest lean‑mass loss seen in some GLP‑1 users. Finally, ongoing professional support—monthly check‑ins with a physician, dietitian, or health coach, tracking of weight, blood pressure, and labs, and prompt adjustment of dose or lifestyle tweaks—provides accountability and early detection of side‑effects. Together, these evidence‑based, patient‑centered strategies turn short‑term results into lasting wellness.
Sustaining the weight‑loss gains achieved with GLP‑1 therapy hinges on three pillars. First, a nutrition plan rich in lean protein ( 0.8‑1.2 g/kg body weight daily), fiber, and healthy fats helps preserve muscle mass while the medication slows gastric emptying and curbs appetite. Second, regular physical activity—especially resistance training 2‑3 times per week—maintains lean body mass, supports metabolic health, and counteracts the modest lean‑mass loss seen in some GLP‑1 users. Finally, ongoing professional support—monthly check‑ins with a physician, dietitian, or health coach, tracking of weight, blood pressure, and labs, and prompt adjustment of dose or lifestyle tweaks—provides accountability and early detection of side‑effects. Together, these evidence‑based, patient‑centered strategies turn short‑term results into lasting wellness.
Putting It All Together for Easy, Sustainable Weight Loss
GLP‑1 receptor agonists such as semaglutide and tirzepatide have proven they can cut appetite, slow gastric emptying, and improve insulin sensitivity, delivering average weight‑loss results of 10‑20 % of baseline body weight while also lowering blood pressure, cholesterol, and diabetes risk. Their safety profile is favorable when patients are screened for thyroid cancer history, pancreatitis, or severe gastrointestinal disease, and common gastrointestinal side effects usually subside after a few weeks of dose titration.
To translate these pharmacologic gains into lasting change, an integrative, personalized plan is essential. Pair the medication with balanced nutrition (adequate protein, fiber, and healthy fats), regular aerobic and resistance exercise, and mind‑body practices such as mindfulness or yoga. Ongoing support from dietitians, health coaches, and behavioral counselors helps patients navigate cravings, manage stress, and preserve lean muscle mass.
Next steps: schedule a comprehensive medical assessment to confirm eligibility (BMI ≥ 30 kg/m² or ≥ 27 kg/m² with comorbidities), discuss any contraindications, and develop a tailored lifestyle blueprint. Commit to weekly follow‑ups for dosage adjustments, side‑effect monitoring, and encouragement—this coordinated, patient‑centered approach maximizes sustainable weight loss and overall well‑being.
