Introduction
Integrative and holistic health blends evidence‑based conventional medicine with complementary therapies—such as acupuncture, yoga, mindfulness, and nutritional counseling—to treat the whole person: body, mind, and spirit. This patient‑centered approach respects individual preferences, cultural beliefs, and lifestyle factors while aiming to improve outcomes, reduce medication side‑effects, and enhance overall well‑being. The purpose of this article is to clarify how these complementary modalities can be safely incorporated alongside standard care, highlight the scientific evidence supporting their use, and guide clinicians and patients toward personalized treatment plans that empower individuals to take an active role in their health journey.
Defining Integrative Medicine and Its Distinction from Conventional Care
| Aspect | Integrative Medicine | Conventional Medicine |
|---|---|---|
| Primary Focus | Whole‑person health (body, mind, spirit, environment) | Disease‑oriented, pathology focus |
| Approach | Multimodal, coordinated plans with multiple providers | Single‑modal, protocol‑driven treatments |
| Patient Role | Active partner in shared decision‑making | Passive recipient of clinician‑directed care |
| Emphasis | Prevention, lifestyle modification, psychosocial factors | Symptom/diagnosis treatment, pharmacologic or surgical interventions |
| Evidence Use | Combines evidence‑based conventional therapies with complementary modalities that have demonstrated efficacy | Relies exclusively on interventions with robust clinical trial evidence |
| Care Coordination | Integrated team (MD/DO, PT, mental‑health, CAM providers) | Often siloed specialties with limited cross‑disciplinary interaction |
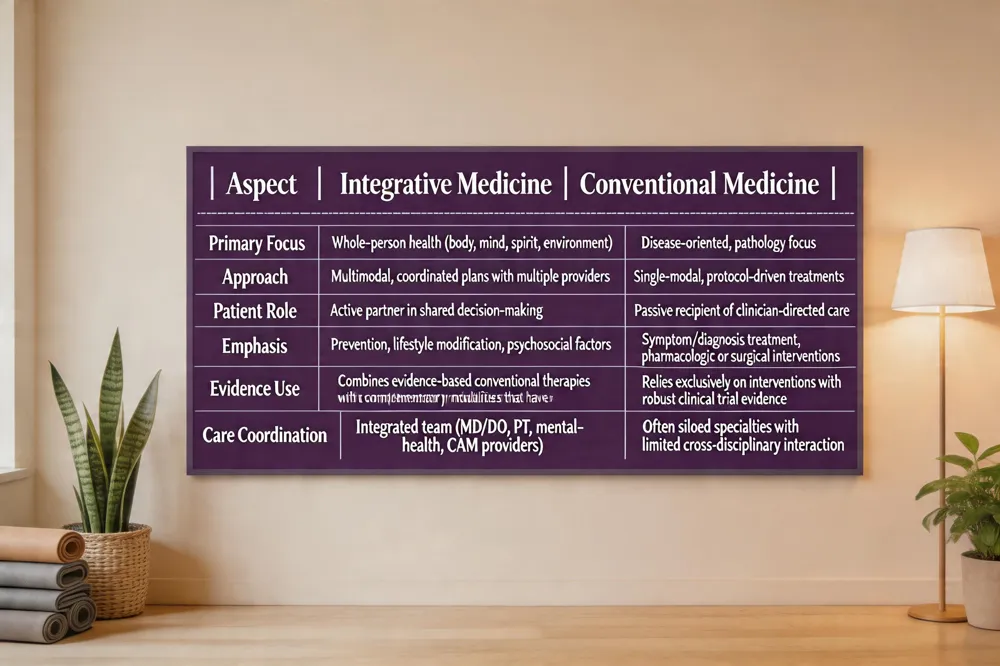 Integrative medicine blends evidence‑based conventional treatments—such as pharmaceuticals, surgery, and physical therapy—with complementary approaches like acupuncture, yoga, mindfulness, and nutritional counseling to address the whole person. Unlike conventional care, which is disease‑oriented and protocol‑driven, integrative care emphasizes prevention, lifestyle modification, and the interconnected biological, behavioral, social, and environmental factors that influence health. It uses coordinated, multimodal plans that involve multiple providers and actively engages patients in shared decision‑making.
Integrative medicine blends evidence‑based conventional treatments—such as pharmaceuticals, surgery, and physical therapy—with complementary approaches like acupuncture, yoga, mindfulness, and nutritional counseling to address the whole person. Unlike conventional care, which is disease‑oriented and protocol‑driven, integrative care emphasizes prevention, lifestyle modification, and the interconnected biological, behavioral, social, and environmental factors that influence health. It uses coordinated, multimodal plans that involve multiple providers and actively engages patients in shared decision‑making.
How does integrative medicine differ from conventional medicine? Integrative medicine intentionally combines proven conventional therapies with complementary modalities to achieve personalized, holistic wellness, whereas conventional medicine focuses primarily on diagnosing and treating pathology with drugs or surgery alone.
Differences between conventional and alternative medicine: Conventional medicine relies on rigorously tested interventions; alternative medicine is used in place of conventional care and often lacks strong evidence. Complementary therapies are used alongside conventional care, while integrative health merges both under a coordinated, patient‑centered model.
Major CAM categories: 1) Mind‑body therapies (meditation, yoga, biofeedback); 2) Biologically based therapies (herbs, vitamins, supplements); 3) Manipulative and body‑based methods (chiropractic, massage, osteopathy); 4) Energy therapies (Reiki, therapeutic touch, qigong); 5) Whole medical systems (Traditional Chinese Medicine, Ayurveda, homeopathy).
Core Concepts: Complementary, Integrative, and Holistic Therapies
| Therapy Type | Definition | Typical Examples |
|---|---|---|
| Complementary | Non‑mainstream practices used alongside standard care to enhance outcomes | Acupuncture, yoga, herbal supplements, chiropractic, aromatherapy, meditation, tai chi |
| Alternative | Practices used instead of conventional care (generally less evidence) | Homeopathy, unproven herbal regimens, certain energy healing without integration |
| Integrative | Merges evidence‑based conventional and complementary approaches under a coordinated, patient‑centered model | MD‑led care plans that include acupuncture, nutrition counseling, mindfulness, and standard medication |
| Holistic | Treats the entire person, overlapping with complementary and integrative modalities | Mind‑body practices, whole‑person counseling, integrative nutrition, spiritual care |
| Mind‑Body | Practices linking mental focus, breath, and movement to affect physiology | Meditation, yoga, tai chi, qigong, guided imagery, mindfulness‑based stress reduction |
 Integrative medicine blends evidence‑based conventional treatments with complementary modalities to create a patient‑centered, whole‑person plan that addresses body, mind, and spirit. Complementary therapies are non‑mainstream practices such as acupuncture, yoga, herbal supplements, chiropractic, aromatherapy, meditation, and tai chi used together with standard care to enhance outcomes or relieve symptoms that drugs alone may not fully address. When these practices replace conventional treatment they are called alternative, a distinction emphasized by the NCCIH. Holistic therapies share the same goal of treating the entire person, often overlapping with complementary approaches (e.g., acupuncture, massage, mindfulness, yoga, herbal medicine). Mind‑body practices—meditation, yoga, tai chi, qigong, guided imagery, mindfulness‑based stress reduction—link mental focus, breath, and movement to lower stress hormones, improve mood, and modulate pain perception. The five C’s of mindfulness—consciousness, compassion, confidence, courage, and community—guide patients toward greater self‑awareness and resilience, supporting the integrative goal of personalized, evidence‑informed care.
Integrative medicine blends evidence‑based conventional treatments with complementary modalities to create a patient‑centered, whole‑person plan that addresses body, mind, and spirit. Complementary therapies are non‑mainstream practices such as acupuncture, yoga, herbal supplements, chiropractic, aromatherapy, meditation, and tai chi used together with standard care to enhance outcomes or relieve symptoms that drugs alone may not fully address. When these practices replace conventional treatment they are called alternative, a distinction emphasized by the NCCIH. Holistic therapies share the same goal of treating the entire person, often overlapping with complementary approaches (e.g., acupuncture, massage, mindfulness, yoga, herbal medicine). Mind‑body practices—meditation, yoga, tai chi, qigong, guided imagery, mindfulness‑based stress reduction—link mental focus, breath, and movement to lower stress hormones, improve mood, and modulate pain perception. The five C’s of mindfulness—consciousness, compassion, confidence, courage, and community—guide patients toward greater self‑awareness and resilience, supporting the integrative goal of personalized, evidence‑informed care.
Mind‑Body Interventions: Definitions, Practices, and Evidence
| Practice | Key Features | Evidence Highlights |
|---|---|---|
| Meditation / MBSR | Focused attention, non‑judgmental awareness, daily practice | Reduces cortisol, improves mood, modest pain reduction in chronic pain trials |
| Yoga | Combined postures, breathwork, meditation | Improves functional mobility, lowers anxiety scores, meta‑analysis shows ↓ pain intensity |
| Tai Chi / Qigong | Slow, flowing movements with breath coordination | Enhances balance, reduces inflammatory markers, effective for osteoarthritis pain |
| Progressive Muscle Relaxation | Systematic tensing/relaxing muscle groups | Lowers sympathetic activity, reduces perceived stress |
| used in peri‑operative settings | ||
| Guided Imagery | Vivid mental visualization of soothing scenes | Improves coping, diminishes procedural anxiety, modest analgesic effect |
| Deep Breathing (Diaphragmatic) | Slow, abdominal breathing patterns | Immediate autonomic shift to parasympathetic dominance, ↓ heart rate variability stress |
| Hypnosis | Suggestion‑based trance state for symptom modulation | Strong evidence for acute procedural pain, chronic low‑back pain relief |
| Biofeedback | Real‑time display of physiological signals (e.g., EMG, HRV) | Trains patients to control muscle tension, effective for migraine and tension‑type headaches |
 What is the definition of mind‑body interventions?
What is the definition of mind‑body interventions?
mind‑body interventions are intentional practices that use mental processes—such as attention, intention, and imagery—to influence physiological functions and promote overall wellness. Classified as complementary health approaches, they are often integrated with conventional care in an integrative health model to support whole‑person health, including chronic pain, anxiety, and stress management.
What are common mind‑body practices?
Common modalities include meditation and mindfulness‑based stress reduction (MBSR), yoga, tai chi, qigong, progressive muscle relaxation, guided imagery, deep‑breathing, hypnosis, and biofeedback. These techniques combine focused attention, gentle movement, and breath control to reduce cortisol, improve autonomic balance, and enhance emotional regulation.
What are the differences between complementary and alternative medicine?
Complementary therapies are used together with conventional treatment (e.g., acupuncture alongside analgesics), whereas alternative therapies replace standard care. The same modality can be either, depending on patient choice and provider guidance, underscoring the need for open discussion with healthcare professionals.
What are the 5 C’s of mindfulness?
Consciousness, compassion, confidence, courage, and community—each fostering present‑moment awareness, kindness, self‑trust, resilience, and supportive practice environments.
What is the mind‑body connection?
A bidirectional link where mental states (stress, emotion) affect neuro‑endocrine, immune, and inflammatory pathways, and physical conditions influence mood and cognition. Integrative care leverages this mind‑body connection to improve pain, mental health, detoxification, and weight‑loss outcomes.
What is the mind‑body controversy?
A philosophical debate on whether mind and body are separate (dualism) or unified (monism). Modern science leans toward integrated models, recognizing mental processes can causally affect physiological health, a premise supported by growing clinical trial evidence. Mind‑body interventions
Evidence‑Based Complementary Therapies for Pain, Mental Health, and Chronic Conditions
| Therapy | Category | Evidence Summary |
|---|---|---|
| Chiropractic Spinal Manipulation | Manipulative & Body‑Based | Systematic reviews show modest benefits for low‑back pain, comparable to standard care |
| Therapeutic Massage | Manipulative & Body‑Based | Reduces muscle tension, improves sleep, short‑term pain relief in musculoskeletal disorders |
| Yoga / Tai Chi / Qigong | Mind‑Body | Improves functional outcomes, lowers pain scores, meta‑analyses support chronic low‑back and knee pain |
| MBSR / Mindfulness | Mind‑Body | Reduces anxiety, depression, and pain catastrophizing; FDA‑cleared for chronic pain adjunct |
| Guided Imagery & PMR | Mind‑Body | Decrease peri‑operative anxiety, improve postoperative pain control |
| Deep Breathing | Mind‑Body | Acute reduction in stress hormones, adjunct for asthma and hypertension |
| Curcumin (Turmeric) | Biologically Based | Anti‑inflammatory, analgesic effects in osteoarthritis; high‑quality RCTs support ↓ pain |
| Omega‑3 Fatty Acids | Biologically Based | Improves inflammatory profile, modest benefit for rheumatoid arthritis pain |
| Magnesium | Biologically Based | Helpful for muscle cramps and migraine prophylaxis; evidence for chronic musculoskeletal pain |
| Ginger | Biologically Based | Anti‑nausea and anti‑inflammatory; RCTs show ↓ pain in osteoarthritis |
| Boswellia Serrata | Biologically Based | Strong anti‑inflammatory, analgesic in chronic low‑back and knee pain |
| Vitamin D | Biologically Based | Deficiency linked to increased pain; supplementation reduces musculoskeletal pain when deficient |
| CBT / ACT | Mental‑Health (Behavioral) | Robust evidence for reducing pain‑related disability and depressive symptoms |
| Hypnosis | Mind‑Body | Effective for acute procedural pain and chronic low‑back pain as adjunct |
| Biofeedback | Mind‑Body | Evidence for migraine, tension‑type headache, and chronic pelvic pain |
 Holistic pain‑management blends conventional care with evidence‑backed modalities that address body, mind, and spirit. Physical approaches such as chiropractic spinal manipulation, therapeutic massage, yoga, Tai Chi, and Qigong improve movement, reduce muscle tension, and modulate nervous‑system signaling. Mind‑body techniques—mindfulness‑based stress reduction, guided imagery, progressive muscle relaxation, and deep‑breathing—lower cortisol, enhance coping, and diminish pain intensity.
Holistic pain‑management blends conventional care with evidence‑backed modalities that address body, mind, and spirit. Physical approaches such as chiropractic spinal manipulation, therapeutic massage, yoga, Tai Chi, and Qigong improve movement, reduce muscle tension, and modulate nervous‑system signaling. Mind‑body techniques—mindfulness‑based stress reduction, guided imagery, progressive muscle relaxation, and deep‑breathing—lower cortisol, enhance coping, and diminish pain intensity.
Natural pain‑relief supplements with robust data include curcumin (turmeric), omega‑3 fatty acids, magnesium, ginger, boswellia serrata, and vitamin D. Curcumin and boswellia show the strongest anti‑inflammatory and analgesic effects; omega‑3s and magnesium aid musculoskeletal discomfort, while adequate vitamin D correlates with reduced chronic pain. All should be used under professional guidance to avoid drug interactions.
Mental‑health therapies for chronic pain that consistently reduce distress and disability are cognitive‑behavioral therapy (CBT), acceptance and commitment therapy (ACT), and mindfulness‑based stress reduction (MBSR). Complementary tools such as hypnosis, biofeedback, and guided relaxation further enhance pain outcomes when integrated into a personalized, patient‑centered plan.
Practical Integration, Insurance, and Emerging Innovations
| Aspect | Details |
|---|---|
| Insurance Coverage | Medicare Part B and many commercial plans reimburse acupuncture, chiropractic, massage, and mindfulness programs (often with physician referral and visit limits). Herbal supplements usually not covered; cash‑pay or discounted‑rate options common. |
| Practical Examples | • Acupuncture + standard analgesics → ↓ opioid dose for chronic back pain<br>• Yoga + psychotherapy → improved anxiety and QoL in cancer survivorship<br>• Nutritional counseling with omega‑3 & vitamin D → adjunct metabolic control in inflammatory disorders |
| Emerging Treatments | • High‑frequency spinal cord & peripheral nerve stimulation (drug‑free pain control)<br>• Platelet‑rich plasma injections for tissue healing<br>• Immersive virtual‑reality distraction for acute procedural pain<br>• Integrated digital platforms combining physical therapy, CBT, and nutrition tracking |
| 5 Major CAM Types | 1) Mind‑Body (meditation, yoga, biofeedback)<br>2) Biologically Based (herbs, vitamins, supplements)<br>3) Manipulative & Body‑Based (chiropractic, osteopathy, massage)<br>4) Energy (Reiki, therapeutic touch, qigong)<br>5) Whole Medical Systems (TCM, Ayurveda, homeopathy) |
 Does insurance cover integrative medicine? Coverage varies by payer and state. Many commercial insurers and Medicare Part B reimburse acupuncture, chiropractic, massage, and mindfulness‑based programs when delivered by licensed providers, often with a limited number of visits and a physician’s referral. Herbal supplements and other whole‑person treatments are less frequently covered and may require cash payment or a “discounted‑rate” arrangement. Patients should verify network status, authorizations, and out‑of‑pocket costs before scheduling.
Does insurance cover integrative medicine? Coverage varies by payer and state. Many commercial insurers and Medicare Part B reimburse acupuncture, chiropractic, massage, and mindfulness‑based programs when delivered by licensed providers, often with a limited number of visits and a physician’s referral. Herbal supplements and other whole‑person treatments are less frequently covered and may require cash payment or a “discounted‑rate” arrangement. Patients should verify network status, authorizations, and out‑of‑pocket costs before scheduling.
What are some practical examples of integrative medicine? Acupuncture paired with standard analgesics can lower opioid needs for chronic back pain. Mindfulness‑based stress‑reduction, yoga, and tai‑chi are combined with psychotherapy to address anxiety and improve quality of life. Nutritional counseling that includes evidence‑based supplements (e.g., omega‑3s, probiotics) complements medical management of metabolic and inflammatory conditions. Multidisciplinary teams—physicians, physical therapists, mental‑health clinicians, chiropractors, and health coaches—coordinate individualized plans for spinal disorders, post‑surgical recovery, and veteran‑related pain.
What are emerging treatments for chronic pain relief? Advanced neuromodulation (high‑frequency spinal cord and peripheral nerve stimulation) offers drug‑free, programmable pain control. Platelet‑rich plasma injections promote tissue healing and reduce inflammation. Immersive virtual‑reality distraction and biofeedback platforms are being used to rewire pain pathways. Integrated programs that blend physical therapies, behavioral interventions, and targeted nutrition are showing promise for sustained multimodal pain management.
What are the 5 major types of complementary and alternative medicine? 1) Mind‑body therapies (meditation, yoga, biofeedback). 2) Biologically based therapies (herbs, supplements, vitamins). 3) Manipulative and body‑based methods (chiropractic, osteopathy, massage). 4) Energy therapies (Reiki, therapeutic touch, qigong). 5) Whole medical systems (Traditional Chinese Medicine, Ayurveda, homeopathy).
Professional Training, Regulation, and Patient Guidance
| Professional Role | Training Pathway | Key Complementary Modalities Integrated |
|---|---|---|
| Integrative Physician (MD/DO) | Standard med school → residency → board certification → fellowship in Integrative Medicine (ABOIM) | Acupuncture, mindfulness, nutrition/supplements, yoga, herbal medicine, biofeedback |
| Physiotherapist (PT) | Accredited PT program → licensure → optional continuing‑education in CAM | Therapeutic massage, yoga, acupuncture (in some jurisdictions), mindfulness, exercise‑based mind‑body techniques |
| Mental‑Health Clinician (Psychologist, Counselor) | Graduate degree + licensure → training in CBT/ACT → optional mindfulness or hypnosis certification | Mindfulness‑based stress reduction, hypnosis, guided imagery, biofeedback |
| CAM Practitioner (e.g., Chiropractor, Acupuncturist) | Accredited CAM program → state licensure → optional integrative medicine courses | Chiropractic adjustments, acupuncture, herbal consultations, energy healing (if certified) |
| Health Coach / Nutritionist | Certified health coach or dietetics program → continuing education in integrative nutrition | Evidence‑based supplements (omega‑3, vitamin D), dietary counseling, lifestyle coaching |
 Integrative physicians are fully licensed MDs or DOs who complete the same rigorous medical school, residency, and board‑certification pathways as conventional doctors. Many then pursue a fellowship in integrative medicine approved by the American Board of Integrative Medicine® (ABOIM) to gain expertise in evidence‑based complementary therapies. While physiotherapy is a mainstream, evidence‑based discipline within conventional care, it is often combined with complementary modalities—such as acupuncture, yoga, or mindfulness—to create a multimodal, whole‑person treatment plan. Complementary therapies used alongside conventional care include acupuncture, aromatherapy, yoga, Tai chi, herbal medicine, therapeutic massage, chiropractic adjustments, and mindfulness‑based meditation, as well as creative approaches like art, music, and guided imagery. Integrative care also draws on five CAM categories: mind‑body, biologically based, manipulatives/body‑based, energy therapies, and whole‑system medical approaches (e.g., Traditional Chinese Medicine). Patients should discuss any complementary therapy with qualified providers, verify practitioner credentials, and use reputable resources—such as NCCIH, NCI, or professional certification boards—to ensure safety, avoid drug interactions, and achieve personalized, patient‑centered wellness.
Integrative physicians are fully licensed MDs or DOs who complete the same rigorous medical school, residency, and board‑certification pathways as conventional doctors. Many then pursue a fellowship in integrative medicine approved by the American Board of Integrative Medicine® (ABOIM) to gain expertise in evidence‑based complementary therapies. While physiotherapy is a mainstream, evidence‑based discipline within conventional care, it is often combined with complementary modalities—such as acupuncture, yoga, or mindfulness—to create a multimodal, whole‑person treatment plan. Complementary therapies used alongside conventional care include acupuncture, aromatherapy, yoga, Tai chi, herbal medicine, therapeutic massage, chiropractic adjustments, and mindfulness‑based meditation, as well as creative approaches like art, music, and guided imagery. Integrative care also draws on five CAM categories: mind‑body, biologically based, manipulatives/body‑based, energy therapies, and whole‑system medical approaches (e.g., Traditional Chinese Medicine). Patients should discuss any complementary therapy with qualified providers, verify practitioner credentials, and use reputable resources—such as NCCIH, NCI, or professional certification boards—to ensure safety, avoid drug interactions, and achieve personalized, patient‑centered wellness.
Conclusion
Integrative health blends evidence‑based conventional treatments with complementary therapies—such as acupuncture, yoga, mindfulness meditation, massage, and nutritional counseling—to address the whole person: body, mind, and spirit. Clinical research shows that these combined approaches can lessen pain, reduce opioid reliance, improve emotional well‑being, enhance functional outcomes, and increase patient satisfaction. By personalizing care plans to each individual’s preferences, lifestyle, and health goals, clinicians can create more sustainable, patient‑centered strategies that respect cultural values and promote active participation in healing. Open, empathetic dialogue between patients and providers is essential; it allows safety concerns, potential interactions, and realistic expectations to be discussed, fostering trust and collaborative decision‑making. Embracing this partnership empowers patients to engage confidently in integrative treatment pathways. Such a collaborative model also aligns with emerging insurance coverage trends, making holistic care more accessible.
