A New Era for Sustainable Weight Management
GLP‑1 receptor agonists mimic the gut hormone glucagon‑like peptide‑1, slowing gastric emptying, increasing satiety, and enhancing glucose‑dependent insulin release. By acting on hypothalamic appetite centers, they reduce caloric intake without drastic dieting, producing average weight losses of 10‑16 % of body weight in 12‑18 months. Until January 2026, all FDA‑approved GLP‑1 obesity therapies were weekly injections such as semaglutide (Wegovy®) and tirzepatide (Zepbound®). The recent launch of the oral semaglutide pill expands access for patients who prefer a non‑injectable option, while delivering comparable efficacy (≈13 % weight loss) and requiring daily dosing on an empty stomach with a 30‑minute fluid‑free window. Despite their pharmacologic power, sustainable outcomes depend on integrative, holistic care. Combining GLP‑1 therapy with personalized nutrition counseling, regular physical activity, stress‑reduction practices, and behavioral support addresses the mind‑body connection that drives long‑term adherence. Patient‑centered programs that monitor metabolic markers, screen for contraindications (e.g., medullary thyroid carcinoma), and adjust dosing collaboratively ensure safety while empowering individuals to achieve and maintain healthier weight trajectories.
Understanding GLP‑1 Therapy: Efficacy, Mechanisms, and Safety
Quick Reference Table
| Therapy (agent) | Delivery | Avg % Weight Loss* (64‑68 wks) | Common GI Side‑Effects | Rare Serious Events | Cardiovascular Benefit |
|---|---|---|---|---|---|
| Semaglutide (injectable) | Weekly injection | 15‑16 % | Nausea, vomiting, diarrhea, constipation, abdominal fullness | Pancreatitis, gallbladder disease, thyroid C‑cell tumor concern | ≈20 % reduction in major CV events |
| Semaglutide (oral) | Daily tablet | 13 % (with diet) | Same as injectable, usually milder | Same as injectable | Similar CV benefit |
| Tirzepatide | Weekly injection | Up to 22 % (high dose) | Similar GI profile | Same as above | CV benefit comparable |
| Liraglutide | Daily injection | 5‑10 % | Mild GI | Same as above | Modest CV benefit |
*Weight‑loss figures are averages from pivotal phase‑3 trials. Individual results vary.
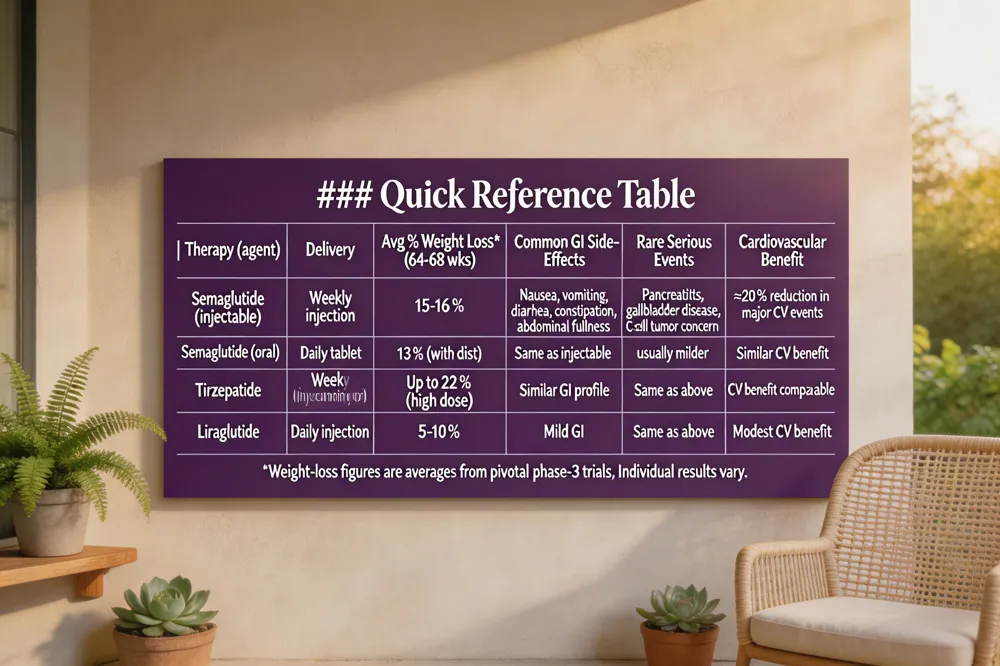 GLP‑1 receptor agonists, whether given as weekly injections (e.g., Wegovy®, Ozempic®) or as the new daily oral tablet, work by mimicking the gut hormone GLP‑1 to slow gastric emptying, increase satiety and modest insulin secretion. Clinical trials show that injectable semaglutide produces an average 15‑16 % body‑weight loss over 64‑68 weeks, while the oral formulation achieves a slightly lower but still impressive 13 % reduction when paired with a reduced‑calorie diet and activity.
GLP‑1 receptor agonists, whether given as weekly injections (e.g., Wegovy®, Ozempic®) or as the new daily oral tablet, work by mimicking the gut hormone GLP‑1 to slow gastric emptying, increase satiety and modest insulin secretion. Clinical trials show that injectable semaglutide produces an average 15‑16 % body‑weight loss over 64‑68 weeks, while the oral formulation achieves a slightly lower but still impressive 13 % reduction when paired with a reduced‑calorie diet and activity.
Short‑term side‑effects are most commonly gastrointestinal—nausea, vomiting, diarrhea, constipation, and abdominal fullness. These symptoms usually lessen after a few weeks of dose titration, and can be mitigated by starting at a low dose, staying well‑hydrated, and adjusting meals. Rare but serious events include pancreatitis, gallbladder disease, and, in patients with a personal or family history of medullary thyroid carcinoma or MEN 2, concerns about thyroid C‑cell tumors.
Long‑term safety appears reassuring: large meta‑analyses have not found a significant increase in cancer incidence, and cardiovascular outcomes are improved (≈20 % reduction in major events). Persistent GI symptoms may lead to dehydration and acute kidney injury if not managed, and clinicians should monitor renal function and thyroid status regularly.
Cancer‑risk surveillance remains part of responsible prescribing. Before initiating therapy, a thorough history for thyroid or pancreatic disease is essential, and periodic monitoring of thyroid function tests is advised. Ongoing research and real‑world registries continue to track rare events, ensuring that the benefits of sustained weight loss outweigh potential risks.
Choosing the Right GLP‑1 Agent for Your Weight‑Loss Goals
Comparative Potency & Cost
| Agent | Formulation | Avg % Weight Loss (clinical) | Potency Rank | Approx. Monthly Cost (self‑pay) | Insurance/Access Notes |
|---|---|---|---|---|---|
| Tirzepatide (Zepbound) | Weekly injection | 22 % (high dose) | 1 (most potent) | $1,200‑$1,500 (injectable) | Prior‑auth common; high‑dose not always covered |
| Semaglutide (Wegovy) | Weekly injection | 15‑21 % | 2 | $1,349 (potentially $675 by 2027) | Often covered for diabetes; obesity indication may need prior‑auth |
| Semaglutide (Rybelsus) | Daily oral tablet | 5‑7 % (obesity studies) | 3 | $299 | FDA‑approved for diabetes; obesity use off‑label |
| Liraglutide (Saxenda) | Daily injection | 5‑10 % | 4 | $900‑$1,200 | Similar coverage challenges as other GLP‑1s |
*Costs are U.S. self‑pay retail prices; patient‑assistance programs may reduce out‑of‑pocket expenses.
 When selecting a GLP‑1 therapy, consider potency, formulation, and cost. Comparative potency – Tirzepatide (Zepbound) currently tops the class, achieving up to 22 % body‑weight loss in trials, followed by high‑dose semaglutide (Wegovy) with 15‑21 % loss. Liraglutide (Saxenda) offers modest 5‑10 % reductions. All three are FDA‑approved for chronic weight management; the choice depends on individual metabolic profile and tolerance. Oral vs injectable – The only oral option in the U.S. is semaglutide (Rybelsus), approved for diabetes but shown to produce 5‑7 % weight loss; higher‑dose oral studies are underway for obesity. Injections (weekly semaglutide or tirzepatide) provide more predictable absorption and greater efficacy, but require needle use. The oral pill must be taken on an empty stomach with strict timing, which can be challenging for some patients. Insurance and cost – Monthly prices range from $299 for the oral Wegovy pill (self‑pay) to $1,349 for the injectable (potentially dropping to $675 by 2027). Many plans cover injections for diabetes but limit obesity indications; prior‑authorization and BMI documentation are often required. Patient‑assistance programs, tele‑health visits, and integrated wellness clinics can reduce out‑of‑pocket expenses. Key take‑aways – Tirzepatide is the most potent injection; oral semaglutide is the best needle‑free choice; no GLP‑1 is available over‑the‑counter. Discuss your health history, lifestyle preferences, and financial situation with a qualified provider to personalize a sustainable, holistic weight‑loss plan.
When selecting a GLP‑1 therapy, consider potency, formulation, and cost. Comparative potency – Tirzepatide (Zepbound) currently tops the class, achieving up to 22 % body‑weight loss in trials, followed by high‑dose semaglutide (Wegovy) with 15‑21 % loss. Liraglutide (Saxenda) offers modest 5‑10 % reductions. All three are FDA‑approved for chronic weight management; the choice depends on individual metabolic profile and tolerance. Oral vs injectable – The only oral option in the U.S. is semaglutide (Rybelsus), approved for diabetes but shown to produce 5‑7 % weight loss; higher‑dose oral studies are underway for obesity. Injections (weekly semaglutide or tirzepatide) provide more predictable absorption and greater efficacy, but require needle use. The oral pill must be taken on an empty stomach with strict timing, which can be challenging for some patients. Insurance and cost – Monthly prices range from $299 for the oral Wegovy pill (self‑pay) to $1,349 for the injectable (potentially dropping to $675 by 2027). Many plans cover injections for diabetes but limit obesity indications; prior‑authorization and BMI documentation are often required. Patient‑assistance programs, tele‑health visits, and integrated wellness clinics can reduce out‑of‑pocket expenses. Key take‑aways – Tirzepatide is the most potent injection; oral semaglutide is the best needle‑free choice; no GLP‑1 is available over‑the‑counter. Discuss your health history, lifestyle preferences, and financial situation with a qualified provider to personalize a sustainable, holistic weight‑loss plan.
Integrating Holistic Strategies with GLP‑1 Therapy
Holistic Components & Key Actions
| Component | Core Actions | Primary Benefits |
|---|---|---|
| Nutrition | Whole‑food, anti‑inflammatory diet; 1,200‑1,500 kcal; eliminate added sugar, gluten, dairy, alcohol, caffeine | Improves gut health, reduces inflammation, supports satiety |
| Movement | Personalized exercise (mix of cardio, strength, flexibility) 150 min/week | Increases energy expenditure, preserves lean mass |
| Sleep | 7‑9 h/night, consistent schedule, limit blue‑light exposure | Hormone balance (leptin, ghrelin), better recovery |
| Stress Management | Mindfulness, yoga, breathing exercises, counseling | Lowers cortisol, reduces emotional eating |
| Supplements (optional) | Apple‑cider‑vinegar capsules, CLA, chromium picolinate, glucomannan (third‑party tested) | May aid appetite control; evidence modest |
| Mental‑Health Support | Therapy, support groups, CBT for eating behaviors | Improves adherence, addresses emotional triggers |
These strategies synergize with GLP‑1‑mediated appetite regulation for sustainable results.
 Is there a holistic approach to weight loss?
Is there a holistic approach to weight loss?
Yes. A whole‑person strategy looks beyond calories and workouts to address hormonal, thyroid, sleep, and emotional factors. It begins with a comprehensive medical evaluation, then builds a personalized nutrition plan centered on whole, unprocessed foods, a tailored movement routine, stress‑reduction practices (mindfulness, yoga, breathing), and support for mental‑health needs such as anxiety or depression. Balance, sustainability, and individualization ensure lasting change and overall well‑being.
14‑day Holistic diet
The first phase eliminates inflammatory foods (added sugars, gluten, dairy, alcohol, caffeine) and emphasizes nutrient‑dense vegetables, fruits, lean proteins, healthy fats, and gluten‑free grains. A short, nutrient‑rich smoothie cleanse follows, giving the digestive system a brief reset. The final phase re‑introduces balanced meals with anti‑inflammatory ingredients and portion sizes of ≈1,200–1,500 kcal, aiming for 2–4 lb weight loss over two weeks. Expert guidance, grocery lists, and community support keep the program realistic and sustainable.
Holistic diet food list
Leafy greens (spinach, kale, chard), whole grains (quinoa, brown rice, oats, millet), healthy fats (avocados, nuts, seeds, olive oil), colorful fruits (berries, oranges, apples), plant‑based proteins (beans, lentils) and high‑quality animal sources (wild‑caught salmon, free‑range poultry, grass‑fed beef) form the foundation of a nutrient‑dense, anti‑inflammatory diet.
Holistic weight‑loss supplements
Natural agents such as apple‑cider‑vinegar capsules, conjugated linoleic acid, chromium picolinate, and glucomannan may aid metabolism and appetite control, but evidence is mixed. Choose third‑party‑tested products and discuss them with a clinician, especially if you have medical conditions or take prescription meds. Supplements should complement—not replace—balanced nutrition, movement, stress management, and adequate sleep.
Holistic weight‑loss medication
Integrative programs combine evidence‑based natural compounds (GLP‑1‑enhancing botanicals, fiber‑rich glucomannan) with personalized lifestyle plans. Under professional supervision, these agents can support metabolism while minimizing side effects, and they work best when paired with sleep optimization, hormone balance, and mental‑health coaching for sustainable results.
Practical Strategies for Sustainable Weight Loss
Actionable Strategies
| Strategy | Description | Typical Outcome |
|---|---|---|
| Calorie Deficit | 500‑750 kcal/day via diet + activity | 1‑2 lb (≈0.5‑1 kg) loss per week |
| Time‑Restricted Eating | 8‑10 h eating window, fasting 14‑16 h | Reduced total intake, improved insulin sensitivity |
| Goal Pairing | Pair weight‑loss target with concrete daily actions (e.g., walk 30 min) | Higher adherence, measurable progress |
| Tracking | Use journal or app for food, activity, weight | Immediate feedback, identifies patterns |
| Professional Coaching | Regular check‑ins with health coach or clinician | Better accountability, early issue detection |
| Avoid Fad Diets | Focus on balanced, nutrient‑dense foods | Long‑term sustainability, reduced rebound weight gain |
Consistent application of these tactics maximizes GLP‑1 benefits while building lasting habits.
 How to lose weight fast naturally and permanently – A modest daily calorie deficit of 500‑750 kcal, achieved through nutrient‑dense whole‑food meals and 150 min of moderate activity weekly, yields a safe 1‑2 lb loss per week. Pair outcome goals (desired weight) with concrete action goals (walk 30 min daily, replace sugary drinks with water). Time‑restricted eating or intermittent fasting can curb intake without extreme restriction. Track intake and activity in a journal or app and enlist support from family, friends, or a health‑coach. Avoid fad diets; steady, balanced changes are far more sustainable.
How to lose weight fast naturally and permanently – A modest daily calorie deficit of 500‑750 kcal, achieved through nutrient‑dense whole‑food meals and 150 min of moderate activity weekly, yields a safe 1‑2 lb loss per week. Pair outcome goals (desired weight) with concrete action goals (walk 30 min daily, replace sugary drinks with water). Time‑restricted eating or intermittent fasting can curb intake without extreme restriction. Track intake and activity in a journal or app and enlist support from family, friends, or a health‑coach. Avoid fad diets; steady, balanced changes are far more sustainable.
Weight loss outcomes, tolerability, side effects, and risks – GLP‑1 receptor agonists (liraglutide, semaglutide, tirzepatide) produce 5‑18 % average weight loss in trials. Common side‑effects are mild‑to‑moderate gastrointestinal symptoms (nausea, diarrhea, constipation, vomiting). Rare serious events include gallbladder disease and acute pancreatitis; delayed gastric emptying may affect anesthesia and colonoscopy preparation. Individualized dosing, thorough assessment, and ongoing monitoring help maximize benefit and mitigate risk.
Benefits of GLP‑1 besides weight loss – GLP‑1s improve glycemic control, lower type 2 diabetes risk, and confer cardiovascular protection (reducing heart attacks, stroke, heart‑failure mortality). They also favorably affect kidney and liver health, reduce joint pain, improve sleep‑apnea severity, and show emerging cognitive benefits. Their influence on gastric emptying and the gut microbiome supports overall metabolic balance.
What I wish I knew before starting GLP‑1 – Early GI upset (nausea, constipation) is common, and some patients experience temporary mental fog or mood changes. Hydration, protein‑rich early meals, and regular sleep help. Regular prescriber‑led check‑ins dramatically improve adherence, and starting with low‑impact exercise prevents early fatigue.
Access, Cost, and Getting Started with GLP‑1 Therapy
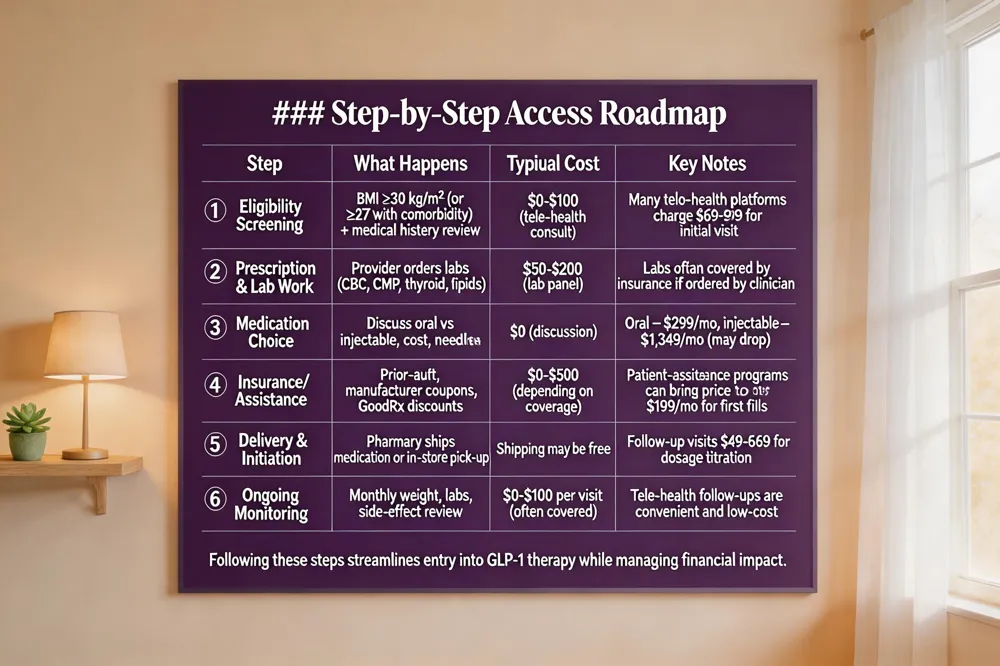
Step‑by‑Step Access Roadmap
| Step | What Happens | Typical Cost | Key Notes |
|---|---|---|---|
| 1️⃣ Eligibility Screening | BMI ≥30 kg/m² (or ≥27 kg/m² with comorbidity) + medical history review | $0‑$100 (tele‑health consult) | Many tele‑health platforms charge $69‑$99 for initial visit |
| 2️⃣ Prescription & Lab Work | Provider orders labs (CBC, CMP, thyroid, lipids) | $50‑$200 (lab panel) | Labs often covered by insurance if ordered by clinician |
| 3️⃣ Medication Choice | Discuss oral vs injectable, cost, needle preference | $0 (discussion) | Cost varies; oral = $299/mo, injectable = $1,349/mo (may drop) |
| 4️⃣ Insurance/Assistance | Prior‑auth, manufacturer coupons, GoodRx discounts | $0‑$500 (depending on coverage) | Patient‑assistance programs can bring price to $199/mo for first fills |
| 5️⃣ Delivery & Initiation | Pharmacy ships medication or in‑store pick‑up | Shipping may be free | Follow‑up visits $49‑$69 for dosage titration |
| 6️⃣ Ongoing Monitoring | Monthly weight, labs, side‑effect review | $0‑$100 per visit (often covered) | Tele‑health follow‑ups are convenient and low‑cost |
Following these steps streamlines entry into GLP‑1 therapy while managing financial impact.
 GLP‑1 medications are prescription‑only drugs, so the first step is to see a qualified clinician who can verify eligibility (BMI ≥ 30 kg/m² or ≥ 27 kg/m² with a weight‑related condition). Many health systems now offer tele‑health visits—Walgreens Weight Management, for example, provides an on‑demand video appointment for $69 and follow‑up chats for $49—allowing a doctor or nurse practitioner to review your health history, order labs, and write a prescription for semaglutide (Wegovy®/Ozempic®), tirzepatide (Zepbound®) or lira... (Saxenda®). After the virtual consult, the pharmacy can ship the medication directly to your home or you can pick it up at a local Walgreens store.
GLP‑1 medications are prescription‑only drugs, so the first step is to see a qualified clinician who can verify eligibility (BMI ≥ 30 kg/m² or ≥ 27 kg/m² with a weight‑related condition). Many health systems now offer tele‑health visits—Walgreens Weight Management, for example, provides an on‑demand video appointment for $69 and follow‑up chats for $49—allowing a doctor or nurse practitioner to review your health history, order labs, and write a prescription for semaglutide (Wegovy®/Ozempic®), tirzepatide (Zepbound®) or lira... (Saxenda®). After the virtual consult, the pharmacy can ship the medication directly to your home or you can pick it up at a local Walgreens store.
Retail pharmacy programs often bundle medication with support services. Walgreens’ online portal lets you start a GLP‑1 regimen, receive counseling, and access limited‑time pricing such as $149 per month for the first two months of Wegovy pills (valid through April 15 2026) or $199 per month for injectables. The injectable Wegovy pen lists at $1,349 per month (potentially dropping to $675 in 2027), while the oral pill costs $299 per month via a self‑pay option.
Insurance coverage varies; many plans require prior authorization and proof of BMI criteria. Patient‑assistance programs, manufacturer coupons, and discount cards (e.g., GoodRx) can lower out‑of‑pocket costs, sometimes to $199 per month for the first fills. Always discuss cost‑saving options with your prescriber and verify that any online or tele‑health provider is state‑licensed to ensure safe, coordinated care.
Putting It All Together: A Patient‑Centric Roadmap
Integrated Patient‑Centric Roadmap
| Phase | Activities | Monitoring | Goal |
|---|---|---|---|
| Evaluation | Full health assessment (BMI, labs, functional‑medicine work‑up) | Baseline weight, blood pressure, thyroid & pancreatic labs | Confirm eligibility & identify contraindications |
| Medication Initiation | Choose oral semaglutide (needle‑free) or injectable (semaglutide/tirzepatide) | Titration schedule, GI symptom log | Achieve target dose with minimal side‑effects |
| Holistic Support | Nutrition counseling, personalized exercise, sleep hygiene, stress‑reduction, mental‑health coaching | Weekly check‑ins (weight, mood, adherence) | Build sustainable lifestyle habits |
| Maintenance | Ongoing dose maintenance, periodic labs, lifestyle reinforcement | Monthly weight/BMI, quarterly labs | Prevent weight regain, maintain metabolic health |
| Long‑Term Success | Support groups, community resources, periodic reassessment of goals | Annual comprehensive review | Continuous improvement in weight, CV health, quality of life |
This roadmap aligns medical therapy with whole‑person care for durable, patient‑centered weight‑loss outcomes.

Sequencing Evaluation, Medication, and Holistic Support
Begin with a comprehensive health assessment—BMI, comorbidities, labs, and a functional‑medicine work‑up—to confirm eligibility (BMI ≥ 30 or ≥ 27 with a weight‑related condition). For patients who prefer a needle‑free option, the newly FDA‑approved oral semaglutide (Wegovy®) offers the same GLP‑1 hormone mimic as the weekly injection. Clinical trials show an average 13 % weight loss over 64 weeks when paired with a reduced‑calorie diet and activity. The pill must be taken on an empty stomach with 4 oz water and no food for 30 minutes; common side effects are nausea, vomiting, diarrhea, or constipation. If injection is preferred, weekly semaglutide (Wegovy) or tirzepatide (Zepbound) provide similar efficacy (15‑16 % loss) and cardiovascular benefits. Complement the medication with personalized nutrition counseling, stress‑reduction practices, and mindful‑eating strategies to address the mind‑body connection.
Monitoring, Adjustments, and Maintenance
Schedule regular check‑ins (monthly or bi‑weekly) to track weight, BMI, blood pressure, and labs. Titrate the dose gradually to minimize gastrointestinal symptoms; most patients see side‑effects wane after the first few weeks. Watch for rare but serious events—gallbladder disease, pancreatitis, or thyroid C‑cell changes—and adjust or discontinue therapy if they arise. Long‑term adherence is crucial; discontinuation typically leads to weight regain, so a maintenance plan that includes ongoing lifestyle coaching is essential.
Resources for Ongoing Success
Leverage tele‑health platforms (e.g., Walgreens Virtual Care, SustainMD) for virtual visits and medication refills. Explore patient‑assist programs to offset the $299‑$1,200 monthly cost of GLP‑1 therapy. Integrative clinics such as the NY Center for Integrative Health provide holistic services—functional labs, IV nutrition, acupuncture—that reinforce medication benefits. Finally, join support groups or counseling to sustain motivation and address emotional eating, ensuring a sustainable, patient‑centered journey toward healthier weight and overall well‑being.
Sustaining Results Through Integrated Care
Long‑term adherence to GLP‑1 therapy hinges on regular monitoring and patient‑centered communication. Clinic visits (or virtual check‑ins) should track weight, BMI, blood pressure, glucose, and gastrointestinal tolerance while screening for rare but serious events such as gallbladder disease or thyroid C‑cell changes. Prompt dose adjustments, counseling on the on empty‑stomach dosing of the oral Wegovy® pill, and reassurance about common nausea or constipation improve persistence; trial data show only 18 % discontinue the oral formulation versus 26 % on placebo.
Beyond medication, sustained weight loss thrives when patients receive continuous lifestyle and holistic support. Integrated programs combine personalized nutrition counseling, mindful‑eating practices, stress‑reduction techniques (yoga, meditation), sleep hygiene, and regular physical activity. Such multimodal care has been shown to preserve a higher proportion of weight loss at 12 months and to mitigate the risk of emotional‑eating relapse.
Future directions include higher‑dose oral semaglutide, combination agents (e.g., bimagrumab with semaglutide), and broader insurance coverage that treats obesity as a chronic disease. Ongoing research on gut‑microbiome modulation, muscle‑preserving adjuncts, and digital dosing tools promises to make GLP‑1 therapy even more effective and patient‑friendly.
