Understanding Outpatient Detox: An Overview
Outpatient detox is a medically supervised withdrawal program that lets patients stay at home while receiving regular clinical visits, medication‑assisted treatment, and vital‑sign monitoring. Safety hinges on a stable living environment, reliable transportation, and a clear plan for rapid escalation if severe symptoms such as seizures or delirium tremens arise. Clinicians conduct an initial medical and psychosocial assessment, then tailor a tapering schedule and medication regimen (e.g., buprenorphine, naltrexone, benzodiazepines) to each individual’s needs. Integrative and holistic therapies—mindfulness meditation, yoga, nutrition counseling, acupuncture, and gentle movement—are increasingly woven into outpatient protocols to address the mind‑body connection, reduce anxiety, and support overall wellness. By combining evidence‑based medicine with personalized, whole‑person care, outpatient detox offers a safe, cost‑effective pathway that preserves work, school, and family responsibilities while laying a solid foundation for long‑term recovery.
What is Detox? The Foundations of Safe Withdrawal
Core Components of Medically Supervised Detox
| Component | Description |
|---|---|
| Initial Assessment | Comprehensive medical, psychiatric, and social evaluation to determine withdrawal risk and appropriate medication plan. |
| Vital‑Sign Monitoring | Continuous checks (BP, HR, temperature, O₂) especially during the first 72 hours to catch seizures, delirium tremens, or dehydration. |
| Laboratory Testing | Baseline labs (CBC, CMP, electrolytes, drug screen) guide medication dosing and detect complications. |
| Medication‑Assisted Treatment (MAT) | Evidence‑based drugs (e.g., benzodiazepines, buprenorphine, naltrexone) to alleviate withdrawal symptoms and prevent life‑threatening events. |
| Holistic Supports | Mindfulness, yoga, nutrition counseling, and acupuncture to promote emotional balance and physical wellness. |
| Crisis‑Line Access | 24/7 phone support for urgent concerns outside scheduled visits. |
| After‑Care Transition | Structured referral to outpatient counseling, peer support, and ongoing MAT to sustain recovery. |
 Detox, short for detoxification, is the body’s process of clearing harmful substances such as alcohol, opioids, or other drugs. In a medical context it is a supervised, systematic withdrawal that manages acute symptoms, reduces health risks, and prepares the patient for continued care. Unsupervised “detox”—often a DIY fasting or juice cleanse—lacks professional monitoring and can be unsafe, especially for substances that can cause seizures, delirium tremens, or severe dehydration.
Detox, short for detoxification, is the body’s process of clearing harmful substances such as alcohol, opioids, or other drugs. In a medical context it is a supervised, systematic withdrawal that manages acute symptoms, reduces health risks, and prepares the patient for continued care. Unsupervised “detox”—often a DIY fasting or juice cleanse—lacks professional monitoring and can be unsafe, especially for substances that can cause seizures, delirium tremens, or severe dehydration.
Medically supervised detox provides continuous vital‑sign monitoring, laboratory testing, and rapid medication‑assisted treatment. A multidisciplinary team—physician, nurses, counselors, and integrative therapists—adjusts medication, offers hydration, nutrition counseling, mindfulness, and yoga to support both physical stabilization and emotional balance. Core components include a thorough initial assessment, individualized medication plan, regular check‑ins, crisis‑line access, and a clear after‑care transition. This patient‑centered, evidence‑based model ensures safety while honoring holistic wellness, creating a stable foundation for long‑term recovery. Insurance coverage is widely available, and telehealth options expand access for rural or busy individuals, reinforcing the program’s flexibility.
Stages of Alcohol Detox and What to Expect
Alcohol Detox Phases & Typical Symptoms
| Phase | Time Frame | Typical Physical Symptoms | Typical Psychological Symptoms | Monitoring Focus |
|---|---|---|---|---|
| Phase 1 | 0‑12 hours | Tremors, anxiety, nausea, sweating, headache | Restlessness, irritability | Vital signs every 2‑4 h; assess for early seizures |
| Phase 2 | 24‑72 hours ("danger zone") | Seizures, visual hallucinations, delirium tremens, high fever | Severe agitation, confusion, panic | Continuous cardiac & neurologic monitoring; adjust MAT |
| Phase 3 | Day 4‑7 → weeks | Decreasing cravings, improved sleep, residual tremors | Mood swings, insomnia, lingering anxiety | Daily check‑ins; focus on relapse prevention and holistic therapy |
 Alcohol detox is usually divided into three phases. Phase 1 (0‑12 hours) brings early signs such as tremors, anxiety, nausea, sweating, and headache as the brain’s hyper‑excitable state begins. Phase 2 (24‑72 hours) is the “danger zone”; symptoms peak and may include seizures, visual‑, and delirium tremens, requiring close medical monitoring. Phase 3 (day 4‑7 and to several weeks) is a post‑acute period where physical cravings fade but sleep disturbances, cravings, mood swings, and lingering anxiety can persist.
Alcohol detox is usually divided into three phases. Phase 1 (0‑12 hours) brings early signs such as tremors, anxiety, nausea, sweating, and headache as the brain’s hyper‑excitable state begins. Phase 2 (24‑72 hours) is the “danger zone”; symptoms peak and may include seizures, visual‑, and delirium tremens, requiring close medical monitoring. Phase 3 (day 4‑7 and to several weeks) is a post‑acute period where physical cravings fade but sleep disturbances, cravings, mood swings, and lingering anxiety can persist.
During a supervised outpatient detox you can expect the initial wave of physical discomfort (muscle aches, sweat, tremors) within the first day, followed by heightened irritability, insomnia, and possible hallucinations in the next few days. Cravings typically peak around days 5‑7, while emotional symptoms may linger for weeks.
Safety is ensured through regular vital‑sign checks, medication‑assisted treatment, and 24/7 crisis support. Integrative tools—mindfulness, nutrition counseling, gentle movement— complement medical care, help stabilize mood, and promote a smoother transition to ongoing therapy.
Outpatient vs Inpatient Detox: Benefits, Payer Preferences, and Ambulatory Care
Outpatient vs. Inpatient Detox Comparison
| Factor | Outpatient (Ambulatory) | Inpatient |
|---|---|---|
| Cost | 30‑50 % cheaper; average $500‑$2,000 vs. $5,000‑$10,000 | Higher due to room/board and 24‑h staffing |
| Length | 7‑14 days (daily/2‑3× weekly visits) can extend 3‑6 months for tapering | 5‑14 days (continuous stay) |
| Monitoring | Scheduled vitals & labs; tele‑health for remote checks | Continuous monitoring (vitals, cardiac, neuro) |
| Ideal Candidates | Stable housing, supportive network, mild‑to‑moderate dependence | High‑risk medical complications, severe withdrawal, lack of support |
| Completion Rate | Often higher (studies show 10‑15 % improvement) | Comparable safety but lower completion for some groups |
| Flexibility | Allows work/school, reduces stigma | Disruptive, requires time away from responsibilities |
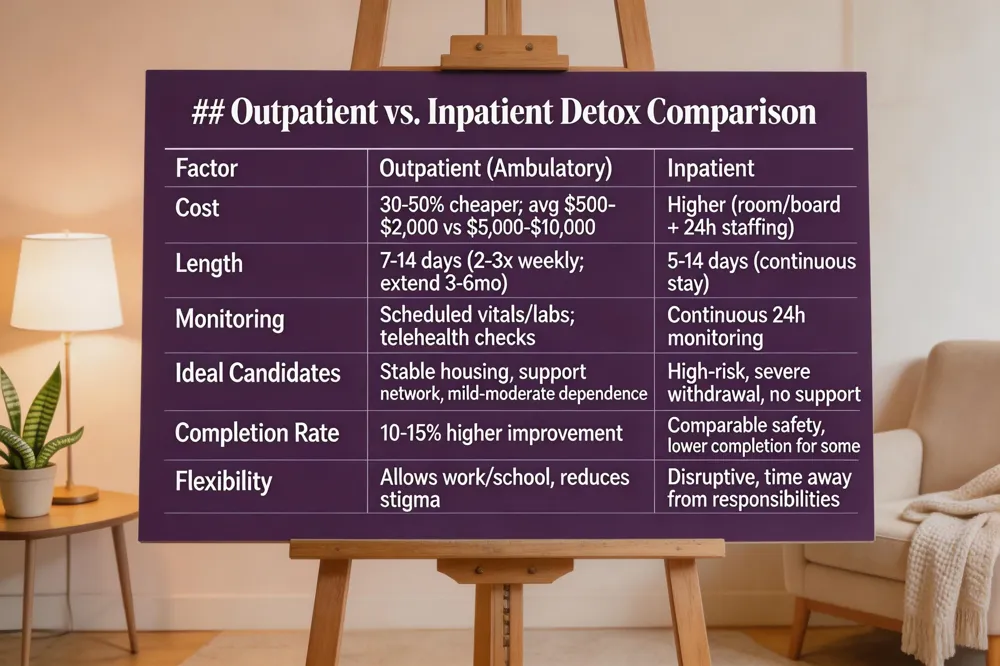 Outpatient detox is dramatically more cost‑effective than inpatient care. By delivering medically supervised withdrawal in a day‑program or telehealth setting, payers avoid overnight room fees, intensive staffing, can the indirect costs of lost work days; insurers therefore favor outpatient routes to keep deductibles, coinsurance and copayments low while preserving hospital capacity. Clinical outcomes for mild‑to‑moderate dependence are comparable across settings: studies show similar safety profiles for visual hallucinations, suicidality and seizures, and higher completion rates in community programs, though severe cases may still benefit from 24‑hour monitoring. Ambulatory detox—also called outpatient detox—provides scheduled clinic visits, medication‑assisted treatment, and optional holistic therapies such as yoga, mindfulness, and nutrition counseling while patients remain at home. Ideal candidates have stable housing, a supportive network, and no high‑risk medical complications, allowing them to maintain work, family and school responsibilities while transitioning smoothly to after‑care counseling and peer support.
Outpatient detox is dramatically more cost‑effective than inpatient care. By delivering medically supervised withdrawal in a day‑program or telehealth setting, payers avoid overnight room fees, intensive staffing, can the indirect costs of lost work days; insurers therefore favor outpatient routes to keep deductibles, coinsurance and copayments low while preserving hospital capacity. Clinical outcomes for mild‑to‑moderate dependence are comparable across settings: studies show similar safety profiles for visual hallucinations, suicidality and seizures, and higher completion rates in community programs, though severe cases may still benefit from 24‑hour monitoring. Ambulatory detox—also called outpatient detox—provides scheduled clinic visits, medication‑assisted treatment, and optional holistic therapies such as yoga, mindfulness, and nutrition counseling while patients remain at home. Ideal candidates have stable housing, a supportive network, and no high‑risk medical complications, allowing them to maintain work, family and school responsibilities while transitioning smoothly to after‑care counseling and peer support.
The Drug Detox Process and Medical Benefits
Drug Detox Process & Medical Benefits
| Step | Action | Example Medications | Primary Benefit |
|---|---|---|---|
| 1️⃣ Assessment | Detailed substance‑use, medical, psychosocial history | N/A | Tailors individualized plan |
| 2️⃣ Medication‑Guided Taper | Gradual dose reduction with MAT | Buprenorphine (opioids), Naltrexone (alcohol), Benzodiazepines (alcohol) | Minimizes withdrawal severity & prevents seizures |
| 3️⃣ Stabilization | Vital‑sign checks, pain/nausea control, hydration | Adjunct meds (anti‑emetics, antipyretics) | Maintains physiological stability |
| 4️⃣ Holistic Integration | Mindfulness, yoga, nutrition, acupuncture | N/A | Improves mood, reduces cravings, supports mind‑body health |
| 5️⃣ Transition Planning | Referral to outpatient therapy, peer groups, ongoing MAT | N/A | Ensures continuity of care and lowers relapse risk |
 Outpatient detox starts with a thorough medical and psychosocial assessment that captures substance‑use history, co‑occurring mental health conditions, and social supports. Clinicians use this information to design a personalized plan that gradually reduces drug levels while prescribing medication‑assisted treatment (MAT) such as buprenorphine for opioid dependence, naltrexone for alcohol, or benzodiazepines for severe alcohol withdrawal. Throughout stabilization, nurses monitor vital signs, manage pain, nausea, anxiety, and prevent complications like seizures or delirium tremens, ensuring safety outcomes comparable to inpatient care. Holistic supports—mindfulness, yoga, nutrition counseling, and acupuncture—are woven into the schedule to address the mind‑body connection and promote overall wellness.
Outpatient detox starts with a thorough medical and psychosocial assessment that captures substance‑use history, co‑occurring mental health conditions, and social supports. Clinicians use this information to design a personalized plan that gradually reduces drug levels while prescribing medication‑assisted treatment (MAT) such as buprenorphine for opioid dependence, naltrexone for alcohol, or benzodiazepines for severe alcohol withdrawal. Throughout stabilization, nurses monitor vital signs, manage pain, nausea, anxiety, and prevent complications like seizures or delirium tremens, ensuring safety outcomes comparable to inpatient care. Holistic supports—mindfulness, yoga, nutrition counseling, and acupuncture—are woven into the schedule to address the mind‑body connection and promote overall wellness.
Drug detox process – Begins with an individualized assessment, follows with a medication‑guided taper, and ends with a transition plan linking to ongoing therapy and peer support.
Benefits of medical detox – Provides 24‑hour clinical oversight, reduces life‑threatening risks, eases physical and emotional symptoms, and lays a stable foundation for long‑term recovery.
Goal of a good detox program – Safely eliminate toxins, stabilize the patient, and connect them to personalized counseling, MAT, and after‑care so they can move confidently toward sustained sobriety and holistic health.
Effectiveness of Outpatient Detox and Patient‑Centric Goals
Effectiveness Metrics & Patient‑Centric Goals
| Metric | Outpatient Findings |
|---|---|
| Completion Rate | 10‑15 % higher than inpatient for mild‑to‑moderate cases |
| Cost Savings | Up to 50 % lower total expense; $500‑$2,000 vs. $5,000‑$10,000 |
| Flexibility | Patients maintain employment, education, family duties |
| Safety Outcomes | Comparable rates of seizures, delirium tremens, and mortality |
| Goal Alignment | • Safe toxin clearance<br>• Stabilize physical & mental health<br>• Immediate link to counseling, MAT, peer support<br>• Empower patient‑centered decision‑making |
 Does outpatient detox work?
Does outpatient detox work?
Outpatient detox is an effective first step for many with mild‑to‑moderate withdrawal when supervised medically. Studies show higher completion rates than inpatient care for such patients, comparable safety outcomes, and lower costs. Success hinges on rapid vitals monitoring, medication‑assisted symptom control, and immediate transition to counseling. Severe dependence or high‑risk medical conditions still merit inpatient care.
What are the benefits of outpatient treatment?
Flexibility lets patients keep work, school, or family duties, reducing disruption and stigma. Cost‑effectiveness saves up to 50 % versus residential stays. Personalized care plans blend CBT, mindfulness, nutrition counseling, and other holistic therapies, allowing practice of coping skills in real‑world settings and fostering stronger support networks.
What is the goal of a good detox program?
The primary aim is safe substance clearance while minimizing withdrawal risk. A good program stabilizes physical and mental health, links patients to after‑care counseling, peer support, and medication‑assisted treatment, and creates a seamless pathway to long‑term recovery that integrates mind‑body wellness and patient‑centered decision‑making.
Practical Considerations: Duration, Costs, and Aftercare Planning
Practical Considerations at a Glance
| Consideration | Details |
|---|---|
| Typical Length – Inpatient | 5‑14 days (most 3‑10 days for acute phase) |
| Typical Length – Outpatient | 7‑14 days (daily/weekly visits) – can extend 3‑6 months for tapering benzodiazepines or methadone |
| Cost Comparison | Outpatient $500‑$2,000 vs. Inpatient $5,000‑$10,000 (30‑50 % cheaper) |
| Insurance Coverage | Medicare, Medicaid, most private insurers, state programs cover medically necessary outpatient detox, including MAT and tele‑health |
| Risks of Unsupervised Detox | Seizures, delirium tremens, severe dehydration, electrolyte imbalance, cardiac/respiratory events, psychiatric crisis |
| After‑Care Importance | Ongoing counseling, peer support, continued MAT → markedly reduces relapse risk and sustains sobriety |
 Typical length of hospital stays and outpatient programs – Inpatient detox usually lasts 5‑14 days, with most facilities keeping patients for 3‑10 days to cover the acute withdrawal window (the first 72 hours are critical for alcohol and opioids). Outpatient detox runs 7‑14 days, often with daily or several‑times‑weekly check‑ins, and can extend to 3‑6 months when tapering benzos or methadone.
Typical length of hospital stays and outpatient programs – Inpatient detox usually lasts 5‑14 days, with most facilities keeping patients for 3‑10 days to cover the acute withdrawal window (the first 72 hours are critical for alcohol and opioids). Outpatient detox runs 7‑14 days, often with daily or several‑times‑weekly check‑ins, and can extend to 3‑6 months when tapering benzos or methadone.
Cost savings and insurance coverage – Outpatient care is 30‑50 % cheaper than inpatient stays (average $500‑$2,000 vs. $5,000‑$10,000). Medicare, Medicaid, most private insurers, and many state programs cover medically necessary outpatient detox, including medication‑assisted treatment and tele‑health visits.
Risks of unsupervised detox and importance of after‑care – Going it alone can trigger seizures, delirium tremens, severe dehydration, or psychiatric crises. Structured after‑care—ongoing counseling, peer support, and, when needed, medication‑assisted treatment—dramatically lowers relapse risk and sustains sobriety.
Key Q&As
- How long is a hospital stay for detox? 5‑14 days, individualized to substance, severity, and health.
- What to expect from a 14‑day detox? Gradual reduction of cravings, improved sleep, modest weight loss, and clearer mental focus, with early‑phase fatigue that eases.
- How can detoxing on your own potentially impact your body? Unmanaged withdrawal can cause seizures, electrolyte imbalance, cardiac events, respiratory complications, and heightened mental‑health distress, raising relapse probability.
Integrating Outpatient Detox into a Holistic Wellness Journey
After the medically supervised withdrawal phase, continuity of care is essential. A seamless transition to outpatient therapy, medication‑assisted treatment, and regular vital‑sign monitoring keeps the body stable while the mind adjusts to sobriety. Personalized after‑care plans are built around each client’s goals, incorporating peer‑support groups, family counseling, and recovery coaching that reinforce motivation and accountability. By aligning these services with integrative health objectives—such as nutrition counseling, yoga, mindfulness meditation, and gentle movement—patients experience a mind‑body synergy that eases cravings, reduces stress, and promotes overall well‑being. This patient‑centered model respects individual preferences, honors cultural values, and provides flexible scheduling ortelehealth options) so treatment fits real‑life responsibilities. When detox is viewed as the first chapter of a broader wellness journey, the combination of evidence‑based medicine and holistic practices creates a stronger, more resilient foundation for lasting recovery.
